Transforming current maternity care starts with education.
Using a transformative framework, we are generating evidence to help influence education standards, curriculum design, programs and professional development opportunities to support the current and future maternity and midwifery workforce.
Trans-Tasman Midwifery Education Consortium Projects
Promoting critical thinking in midwifery students
An extensive body of research work has been undertaken to measure and evaluate the development of critical thinking in undergraduate midwifery students.
Study 1 – Measurement of Critical Thinking in Midwifery
The tools can be used to map critical thinking development across the course of the degree, providing targeted feedback to students, highlighting areas for further development. Although the tools and model were originally designed for use within midwifery students they could also be used with midwives in practice, particularly with newly qualified midwives.
A number of national and international universities are interested in using the CACTiM tools in their undergraduate midwifery program and undertake collaborative research comparing critical thinking development between institutions. If you are interested in using any or all of the CACTiM tools and/ or participating in collaborative research, please contact Dr Amanda Carter. Dr Carter will provide a copy of the tools and guidelines for use.
Publications
Carter, A. G. Critical thinking (2020). In E. Jefford & J. Jomeen (Eds.), Empowering Decision-Making in Midwifery. London: Routledge https://doi.org/10.4324/9780429398179
Carter, A. G., Creedy, D.K. & Sidebotham, M. (2018). Measuring critical thinking in pre-registration midwifery students: A multi-method approach. Nurse Education Today, 61, 169-174.
Carter, A. G., Creedy, D. K., & Sidebotham, M. (2017). Critical thinking evaluation in reflective writing: Development and testing of Carter Assessment of Critical Thinking in Midwifery (Reflection). Midwifery, 54, 73-80.
Carter, A. G., Creedy, D. K., & Sidebotham, M. (2017). Critical thinking skills in midwifery practice: Development of a self-assessment tool for students. Midwifery, 50, 184-192.
Carter, A. G., Creedy, D.K., & Sidebotham, M. (2016). Efficacy of teaching methods used to develop critical thinking in nursing and midwifery undergraduate students: A systematic review of the literature. Nurse Education Today, 40, 209-218
Carter, A.G., Creedy, D.K. & Sidebotham, M. (2016). Development and psychometric testing of the Carter Assessment of Critical Thinking in Midwifery (Preceptor/Mentor version). Midwifery, 34, 141-9.
Carter, A.G., Creedy, D.K. & Sidebotham, M. (2015). Evaluation of tools used to measure critical thinking development in nursing and midwifery undergraduate students: A systematic review. Nurse Education Today, 35(7), 864-874.
Carter, A.G., Sidebotham, M., Creedy, D.K, Fenwick, J. & Gamble, J. (2015). Strengthening partnerships: The involvement of health care providers in the evaluation of authentic assessment within midwifery undergraduate education. Nurse Education in Practice, 15(4), 327-332.
Carter, A. G., Sidebotham, M., Creedy, D. K., Fenwick, J., & Gamble, J. (2014). Using root cause analysis to promote critical thinking in final year Bachelor of Midwifery students. Nurse Education Today, 34(6), 1018-1023.
Lead: Dr Amanda Carter
Dr Amanda Carter’s thesis >
Contact
Study 2 – Conceptual Model of Critical Thinking in Midwifery
This model presents a new understanding of critical thinking in midwifery practice. This staged conceptual model can embedded into midwifery curriculum and be used as a framework to teach and facilitate the development of critical thinking in midwifery. The model can also be used by students, newly qualified or experienced midwives to guide midwifery decision making.
Publications
Carter, A. G., Creedy, D. K., & Sidebotham, M. (2018). Critical thinking in midwifery practice: A conceptual model. Nurse Education in Practice, 33, 114-120.
Lead: Dr Amanda Carter
Study 3 – Development of a Consensus Definition of Critical Thinking in Midwifery: A Delphi Study
Midwives require well developed critical thinking skills to inform professional judgement that is evidence based, safe, woman-centred and individualised. Currently there is no discipline specific definition of critical thinking in midwifery practice. This study using a Delphi technique will develop an international consensus definition of critical thinking in midwifery. Midwives recognised as experts in midwifery education, practice, and research from diverse geographical, cultural, and practice areas will be invited to participate in this study. If you would like volunteer to contribute to this Delphi study please contact Dr Amanda Carter.
Lead: Dr Amanda Carter
Developing reflective capacity in midwifery students
Using Education Design Research (EDR) methodology as the framework for this Doctoral study, this project aims to develop and evaluate educational tools and strategies to facilitate the development of reflective capacity in midwifery students.
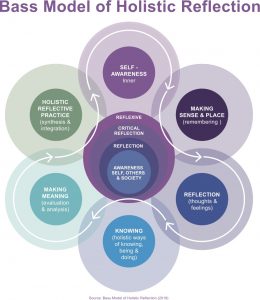
The first two phases of the project are complete including an educational needs and conceptual analysis with integrative review of the literature. This informed the design and development of a structured model of holistic reflection for use in midwifery – the Bass Model (Bass et al, 2017).
The third phase involved a pilot of the utility of the Bass Model of Holistic Reflection using a cross sectional collaborative study involving midwifery students enrolled in pre-registration midwifery programs at two Universities (Bass et al, 2019; Sweet, Bass et al, 2018). The findings from this study informed development of education resources for midwifery students to support development of reflective capacity and a tool to assess reflective writing skills.
Phase Four explored the education needs of facilitators who support development of reflective capacity in midwifery students. This informed development of a Reflective Practice Toolkit for educators. The findings from this study have been submitted to Nurse Education in Practice November 2019.
Phase Five is currently in progress and involves development of a validated Reflective Inventory for use by midwifery students and educators to assess development of holistic reflective capacity. The final phase will include evaluation of effectiveness of the Bass Model in promoting the development of holistic reflective capacity in midwifery students.
Co-Leads: Janice Bass (PhD candidate) with Associate Professor Mary Sidebotham, Professor Debra Creedy, and Professor Linda Sweet from Deakin University
Collaborating partners: School of Nursing and Midwifery Flinders University, School of Midwifery, Auckland University of Technology
Contact
Publications:
Bass, J., Fenwick. J., & Sidebotham, M. (2017). Development of a Model of Holistic Reflection to facilitate transformative learning in student midwives. Women and Birth 30(3), 227 – 235.
Bass, J., Sidebotham, M., Creedy, DK. & Sweet, L. (2020). Midwifery students’ experiences and expectations of using a model of holistic reflection. Women and Birth, 33(4), 383-392.
Sweet, L., Bass, J., Sidebotham, M., Fenwick, J., & Graham, K. (2018). Developing reflective capacities in midwifery students: Enhancing learning through reflective writing. Women and Birth, 32(2), 119-126.
Sweet, L., Bass, J., & Graham, K. (2019). The Continuity of Care Experience and Reflective Writing: Enhancing Post-Practicum Learning for Midwifery Students. In Augmenting Health and Social Care Students’ Clinical Learning Experiences (Vol. 25, pp. 141-162). (Professional and Practice-based Learning; Vol. 25). Springer, Cham.
Bass, J. Sweet,L. Creedy, DK., & Sidebotham, M. (2020). Exploring the needs and experiences of educators in facilitating use of the Bass Model of Holistic Reflection. Nurse Education in Practice, 46, 102805.
Optimising the clinical education experience
These projects involve designing and evaluating innovative approaches to clinical education for pre-registration midwifery programs.
Study 1 – Evaluation of clinical learning environment (MidSTEP)
It is known that the quality of clinical practice experience directly impacts student learning.
This study involves developing and evaluating a specific tool to measure the experience of midwifery students during their clinical education: the Midwifery Student Evaluation of Practice (MidSTEP) tool.
As second step, Trans-Tasman Midwifery Education Consortium partners are using the MidSTEP with students enrolled in their university’s midwifery program. This will provide an opportunity to benchmark across programs and countries (Australia and New Zealand). We expect MidSTEP to be a valuable tool for the international midwifery education community and will seek for it to be incorporated into the standards governing midwifery education programs.
Lead: Marnie Griffiths
Contact: Marnie Griffiths to discuss use of the MidStep tool
Collaborating partners: Flinders University, University of South Australia, Auckland University of Technology, University of Technology Sydney, University of Canberra.
Study 2 – Promoting the quality of clinical education by midwifery preceptor
Clinical learning environments are critical to the preparation of midwives for skill development, professional identity, and confidence as a midwife. Registered midwives, as preceptors, play a key role in clinical learning environments. Unlike clinical nursing, midwifery reflects a social model of healthcare, is holistic, and inclusive of women’s preferences and values.
This study aims to contribute to the optimisation of midwifery clinical education by:
- developing and testing a measure of preceptors’ perceptions of quality midwifery clinical education
- developing a novel preceptor program
- evaluating the program’s impact using Kirkpatrick’s Levels of Learning
Publications:
Griffiths, M., Creedy, D., & Carter, A. (2020). Validation of the MidACE tool – Student’s perceptions of the Midwifery Academic role in clinical environments. Women and Birth, in press.
Co-leads: Marnie Griffiths (PhD student) with Professor Debra Creedy and Dr Amanda Carter
Contact
Study 3 – Hearing women’s voices: promoting active learning within the continuity of midwifery care experience
This project consists of three phases, including:
- Surveying women who have received continuity of midwifery care from a midwifery student in order to measure satisfaction with care provided
- Comparing aggregated clinical outcome data from the midwifery student’s clinical e-portfolios with national perinatal data.
- Integrating women’s feedback into midwifery students’ clinical assessment
Lead: Professor Jenny Gamble
Contact
Study 4 – Evaluation of midwifery caseload model for midwifery students
Griffith University recognises the value of continuity of care experiences and therefore requires midwifery students to undertake a minimum of 20 continuity of care experiences across their degree program.
In 2018, Midwifery@Griffith, in partnership with one of their primary practice partners, the Gold Coast University Hospital (GCUH), introduced an extended six-month caseload placement for interested 3rd Year midwifery students.

In 2019, we have built on this initiative and provided extended caseload placement for midwifery students at Gold Coast University Hospital, Logan Community Maternal and Child Health Hubs, Beaudesert Midwifery Group Practice, and Redland Midwifery Group Practice.
The aim of this study is to evaluate the outcomes of embedding students within the caseload practice where they work in a continuity of care model alongside a known midwife for six months. During this time the student will recruit 10 continuity of care experiences within the caseload.
Analysis of data is in progress and findings are being written up.
Co-Leads: Associate Professor Kathleen Baird and Carolyn Hastie
Contact
Study 5 – The impact on learning of student-led caseload clinics
A clinical environment that provides meaningful and productive learning experiences is essential for students of all health care professions. To support the learning needs of undergraduate midwifery students and facilitate the continuity of care experiences a student led clinic was established in one South East Queensland maternity unit. This study explored the experiences and learning processes of student midwives undertaking clinical practice within this student led clinic.
A qualitative descriptive approach was used. Ten students that worked in the clinic were invited to participate in a one off digitally recorded face to face or telephone interview. Thematic analysis was used to analyse the data set. University ethical approval was granted.
Preliminary findings suggest that the student led clinic placed students in ‘the driver’s seat’. Overwhelmingly students described the clinic as providing them with an array of opportunities to ‘lead’ care rather than being forced to ‘sit and watch’. The central elements of the experience were having more time to be holistic in their approach, development of enhanced skills, getting to know the woman through the continuity of care relationship and feeling supported, by their university practice lectures, to bridge the theory – practice gap. Students perceived that the experience of working in the clinic increased their midwifery knowledge, skills, confidence, critical thinking, care planning, and ability to advocate for and empower women.
High quality and supportive clinical teaching and learning experiences are vital for ensuring the student midwife develops into a competent practitioner who is fit for registration. The evidence from this small study highlights the benefits afforded to students of working in partnership not only with pregnant women but also with their university midwifery lecture. The student’s continuity of care learning experiences appeared to foster and cultivate their capability, identity, purpose, resourcefulness and connection; all the five senses of success.
Publications: Hamilton, Baird, Fenwick. (2019). Nurturing autonomy in student midwives within a student led antenatal clinic. Women and Birth, 33(5), 448-454. https://doi.org/10.1016/j.wombi.2019.12.001
Co-Leads: Valerie Hamilton (Masters research), Professor Kathleen Baird and Adjunct Professor Jennifer Fenwick
Contact
Study 6 – Optimising the use of technology to support clinical learning
Within the Bachelor of Midwifery program at Griffith University we use an interactive e-portfolio (M@GIE) to support students clinical learning. M@GIE is highly accessible and integrated tool for measuring diverse aspects of student learning, progress and achievement. We are refining and enhancing the functionality of M@GIE and planning studies on impact and value as a learning tool. We would welcome partners for this ongoing work.
Lead: Marnie Griffiths
Contact
Study 7 – Enhancing students’ clinical learning in continuity of midwifery care models: Evaluating a quality improvement strategy
Women-centred continuity of midwifery care (CMC) is essential to safe and quality maternity care. However, midwifery students do not currently integrate women’s feedback or clinical outcomes into their clinical assessment. This program of work will place the women receiving CMC from a midwifery student in the clinical learning and assessment cycle. The strong emphasis on CMC and woman-centred care prepares midwifery graduates to work to their full scope of practice, and be critically reflective practitioners. Expanding the functionality of the student e-portfolio to capture women’s feedback and enable easy analysis of clinical data prepares midwifery graduates for registration and gather data as part of their ongoing endorsement. This program will also benefit future Bachelor of Midwifery (BMid) students by providing ongoing improvements to the clinical ePortfolio used within the BMid program as well as more robust and meaningful improvements to clinical assessment. Women will benefit from a workforce of graduate midwives who not only seek women’s ongoing feedback but know how to respond to feedback and change practice accordingly.
Publications: Tickle, N., Sidebotham, M., Fenwick, J. & Gamble, J. (2016). Women’s experiences of having a Bachelor of Midwifery student provide continuity of care. Women and Birth, 29 (3), 245-251. https://doi.org/10.1016/j.wombi.2015.11.002
Co-leads: Nikki Tickle, Professor Jenny Gamble, Professor Debra Creedy
Study 8 – Enhancing awareness of cultural safety among midwifery academics
The ultimate aim of this program of research was to help build a midwifery workforce that is profoundly aware of the importance of being culturally safe. The PhD project aimed to improve awareness of Cultural Safety amongst midwifery academics. The provision of culturally safe educational experiences and learning and teaching practices are key strategies to improving the academic success of First Peoples students.
The research project included 6 studies:
- An integrative systematic review of educational strategies to promote academic success and resilience in undergraduate Indigenous students.
- A second integrative review of the literature on the scope and efficacy of professional development interventions to increase awareness of Cultural Safety by midwifery academics.
- The development of a tool measuring awareness of Cultural Safety.
- Implementation and evaluation of a continuing professional development intervention to improve midwifery academics’ awareness of Cultural Safety.
- An exploration of the impact of yarning circles within a professional development program to enhance midwifery academics’ awareness of Cultural Safety.
- The final study examined awareness of Cultural Safety within the broader midwifery profession.
Conceptual Model – achieving Cultural Safety through a reframed Standpoint Theory
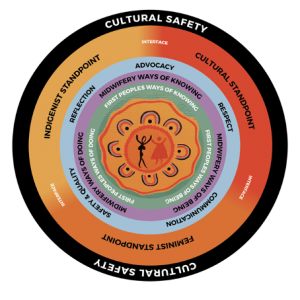
To make such a paradigm shift and adopt a decolonised lens, a reframed standpoint approach was conceptualised. The reframed standpoint was an interpretation only and came from a place of deep respect and desire to understand complex concepts associated with Cultural Safety, new knowledge, and ways of knowing. The reframed standpoint approach used alongside the five capabilities of The Framework (Department of Health, 2015a) were instrumental in providing guidance throughout this body of work by weaving together, the capabilities (respect; communication; safety and quality; reflection; advocacy).
Acknowledgement is made to Kim Williams (Brolga), artist and proud Kullilli-Wakka-Wakka woman for sharing a piece of her work for the centre of the conceptual model. Beaudesert, Qld, Australia.
Publications
Fleming T., Creedy, D., & West, R. (2019). The influence of yarning circles: A Cultural Safety professional development program for midwives. Women and Birth, 33(2), 175-185. https://doi.org/10.1016/j.wombi.2019.03.016
Fleming T., Creedy, D., & West, R. (2018). Awareness of cultural safety in the Australian midwifery workforce: A snapshot. Women and Birth, 32(6), 549-557. https://doi.org/10.1016/j.wombi.2018.11.001
Fleming T., Creedy, D., & West, R. (2018). Cultural safety continuing professional development for midwifery academics: An integrative literature review. Women and Birth, 33(4), 318-326. https://doi.org/10.1016/j.wombi.2018.10.001 (Awarded Caroline Homer Writers Award – runner up 2018).
Fleming, T., Creedy, D., & West, R. (2017). Impact of a continuing professional development intervention on midwifery academics’ awareness of cultural safety. Women and Birth, 30(3), 245-252. http://dx.doi:10.1016/j.wombi.2017.02.004 (Awarded Health group, Griffith University – Publication of the year)
West, R., Gamble, J., Kelly, J., Fleming, T., Duff, E. & Sidebotham, M. (2016). Culturally capable and culturally safe: Caseload care for Indigenous women by Indigenous midwifery students. Women and Birth, 29(6), 524-530.
https://doi.org/10.1016/j.wombi.2016.05.003
Milne, T., Creedy, D., West, R. (2016). Development of the Awareness of Cultural Safety Scale: A pilot study with midwifery and nursing academics. Nurse Education Today, 44, 20-25. https://doi.org/10.1016/j.nedt.2016.05.012
Milne, T., Creedy, D., West, R. (2015). Integrated systematic review on educational strategies that promote academic success and resilience in undergraduate Indigenous students. Women and Birth, 29(6), 524-530. http://dx.doi.org/10.1016/j.wombi.2016.05.003
Lead: Dr Tania Fleming
Evaluating the willingness of new midwives to work in continuity of care models
Study 1 – How motivated, capable and willing are entry to practice midwives in Australia to work in continuity of midwifery care models?
The Australian national midwifery education standards provide a framework to ensure entry to practice programs prepare graduates for contemporary midwifery practice.
The evidence to support the wide-scale implementation of midwifery continuity of care models is irrefutable and therefore, a goal for entry-to-practice programs should be to prepare graduates for this model.
This program of work surveys midwives exiting entry to practice programs to understand their motivation, willingness and level or preparedness to work in continuity of midwifery care models on graduation.
This project is also relevant to the Practice Translation and Workforce Programs.
Lead: Professor Mary Sidebotham
Contact
Publications
Carter, J., Dietsch, E., & Sidebotham, M. (2020). The impact of pre-registration education on the motivation and preparation of midwifery students to work in continuity of midwifery care: An integrative review. Nurse Education in Practice, 48, 102859. https://doi.org/10.1016/j.nepr.2020.102859